Abstract
Background
Ultra-trail running races pose appreciable physiological challenges, particularly for glucose metabolism. Previous studies that yielded divergent results only measured glycaemia at isolated times.
Objectives
We aimed to explore the impact of an ultra-endurance race on continuously measured glycaemia and to understand potential physiological mechanisms, as well as the consequences for performance and behavioural alertness.
Methods
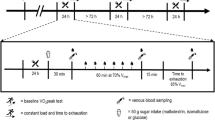
Fifty-five athletes (78% men, 43.7 ± 9.6 years) ran a 156-km ultra-trail race (six 26-km laps, total elevation 6000 m). Participants wore a masked continuous glucose monitoring sensor from the day before the race until 10 days post-race. Blood was taken at rest, during refuelling stops after each lap, and after 24-h recovery. Running intensity (% heart rate reserve), performance (lap times), psychological stress, and behavioural alertness were explored. Linear mixed models and logistic regressions were carried out.
Results
No higher risk of hypo- or hyperglycaemia was observed during the exercise phases of the race (i.e. excluding stops for scientific measurements and refuelling) compared with resting values. Laps comprising a greater proportion of time spent at maximal aerobic intensity were nevertheless associated with more time > 180 mg/dL (P = 0.021). A major risk of hyperglycaemia appeared during the 48-h post-race period compared with pre-race (P < 0.05), with 31.9% of the participants spending time with values > 180 mg/dL during recovery versus 5.5% during resting. Changes in circulating insulin, cortisol, and free fatty acids followed profiles comparable with those usually observed during traditional aerobic exercise. However, creatine phosphokinase, and to a lesser extent lactate dehydrogenase, increased exponentially during the race (P < 0.001) and remained high at 24-h post-race (P < 0.001; respectively 43.6 and 1.8 times higher vs. resting). Glycaemic metrics did not influence physical performance or behavioural alertness.
Conclusion
Ultra-endurance athletes were exposed to hyperglycaemia during the 48-h post-race period, possibly linked to muscle damage and inflammation. Strategies to mitigate muscle damage or subsequent inflammation before or after ultra-trail races could limit recovery hyperglycaemia and hence its related adverse health consequences.
Trial Registration Number
NCT05538442 2022–09-21 retrospectively registered.
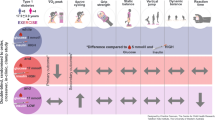
Graphical abstract






Similar content being viewed by others
References
Zaryski C, Smith DJ. Training principles and issues for ultra-endurance athletes. Curr Sports Med Rep. 2005;4(3):165–70.
Hoppel F, Calabria E, Pesta D, Kantner-Rumplmair W, Gnaiger E, Burtscher M. Physiological and pathophysiological responses to ultramarathon running in non-elite runners. Front Physiol. 2019;10:1300.
Ramos-Campo DJ, Avila-Gandia V, Alacid F, Soto-Mendez F, Alcaraz PE, Lopez-Roman FJ, et al. Muscle damage, physiological changes, and energy balance in ultra-endurance mountain-event athletes. Appl Physiol Nutr Metab. 2016;41(8):872–8.
Waskiewicz Z, Klapcinska B, Sadowska-Krepa E, Czuba M, Kempa K, Kimsa E, et al. Acute metabolic responses to a 24-h ultra-marathon race in male amateur runners. Eur J Appl Physiol. 2012;112(5):1679–88.
Millet GY, Tomazin K, Verges S, Vincent C, Bonnefoy R, Boisson RC, et al. Neuromuscular consequences of an extreme mountain ultra-marathon. PLoS One. 2011;6(2): e17059.
Vassalle C, Piaggi P, Weltman N, Prontera C, Garbella E, Menicucci D, et al. Innovative approach to interpret the variability of biomarkers after ultra-endurance exercise: the multifactorial analysis. Biomark Med. 2014;8(6):881–91.
DuBose SN, Li Z, Sherr JL, Beck RW, Tamborlane WV, Shah VN. Effect of exercise and meals on continuous glucose monitor data in healthy individuals without diabetes. J Diabetes Sci Technol. 2021;15(3):593–9.
Ishihara K, Uchiyama N, Kizaki S, Mori E, Nonaka T, Oneda H. Application of continuous glucose monitoring for assessment of individual carbohydrate requirement during ultramarathon race. Nutrients. 2020;12(4):1121.
Kinrade EJ, Galloway SDR. Dietary observations of ultra-endurance runners in preparation for and during a continuous 24-h event. Front Physiol. 2021;12: 765888.
Yardley JE, Colberg SR. Update on management of type 1 diabetes and type 2 diabetes in athletes. Curr Sports Med Rep. 2017;16(1):38–44.
Evans ML, Pernet A, Lomas J, Jones J, Amiel SA. Delay in onset of awareness of acute hypoglycemia and of restoration of cognitive performance during recovery. Diabetes Care. 2000;23(7):893–7.
Heller S, Houwing N, Kragh N, Ploug UJ, Nikolajsen A, Alleman CJ. Investigating the evidence of the real-life impact of acute hyperglycaemia. Diabetes Ther. 2015;6(3):389–93.
Joy NG, Perkins JM, Mikeladze M, Younk L, Tate DB, Davis SN. Comparative effects of acute hypoglycemia and hyperglycemia on pro-atherothrombotic biomarkers and endothelial function in non-diabetic humans. J Diabetes Complications. 2016;30(7):1275–81.
Goel R, Majeed F, Vogel R, Corretti MC, Weir M, Mangano C, et al. Exercise-induced hypertension, endothelial dysfunction, and coronary artery disease in a marathon runner. Am J Cardiol. 2007;99(5):743–4.
De Bosscher R, Dausin C, Claus P, Bogaert J, Dymarkowski S, Goetschalckx K, et al. Lifelong endurance exercise and its relation with coronary atherosclerosis. Eur Heart J. 2023;44(26):2388–99.
Dores H, de Araujo GP, Monge J, Costa R, Tata L, Malhotra A, et al. Subclinical coronary artery disease in veteran athletes: is a new preparticipation methodology required? Br J Sports Med. 2020;54(6):349–53.
Lechner K, Spanier B, Lechner B, Scherr J. Your athlete-patient has a high coronary artery calcification score-’Heart of Stone’. What should you advise? Is exercise safe? Br J Sports Med. 2021;55(18):1001–2.
Scheer V, Tiller NB, Doutreleau S, Khodaee M, Knechtle B, Pasternak A, et al. Potential long-term health problems associated with ultra-endurance running: a narrative review. Sports Med. 2022;52(4):725–40.
Kirwan JP, Hickner RC, Yarasheski KE, Kohrt WM, Wiethop BV, Holloszy JO. Eccentric exercise induces transient insulin resistance in healthy individuals. J Appl Physiol (1985). 1992;72(6):2197–202.
Gonzalez-Ortiz M, Martinez-Abundis E, Balcazar-Munoz BR, Pascoe-Gonzalez S. Effect of sleep deprivation on insulin sensitivity and cortisol concentration in healthy subjects. Diabetes Nutr Metab. 2000;13(2):80–3.
Baur DA, Bach CW, Hyder WJ, Ormsbee MJ. Fluid retention, muscle damage, and altered body composition at the Ultraman triathlon. Eur J Appl Physiol. 2016;116(3):447–58.
Bratusch-Marrain PR. Insulin-counteracting hormones: their impact on glucose metabolism. Diabetologia. 1983;24(2):74–9.
Marliss EB, Vranic M. Intense exercise has unique effects on both insulin release and its roles in glucoregulation: implications for diabetes. Diabetes. 2002;51(Suppl 1):S271–83.
Rand JS, Kinnaird E, Baglioni A, Blackshaw J, Priest J. Acute stress hyperglycemia in cats is associated with struggling and increased concentrations of lactate and norepinephrine. J Vet Intern Med. 2002;16(2):123–32.
Mauvieux B, Hingrand C, Drigny J, Hodzic A, Baron P, Hurdiel R, et al. Study of the kinetics of the determinants of performance during a mountain ultramarathon: multidisciplinary protocol of the first trail Scientifique de Clecy 2021. JMIR Res Protoc. 2022;11(6): e38027.
Battelino T, Danne T, Bergenstal RM, Amiel SA, Beck R, Biester T, et al. Clinical targets for continuous glucose monitoring data interpretation: recommendations from the international consensus on time in range. Diabetes Care. 2019;42(8):1593–603.
Battelino T, Alexander CM, Amiel SA, Arreaza-Rubin G, Beck RW, Bergenstal RM, et al. Continuous glucose monitoring and metrics for clinical trials: an international consensus statement. Lancet Diabetes Endocrinol. 2023;11(1):42–57.
Shah VN, DuBose SN, Li Z, Beck RW, Peters AL, Weinstock RS, et al. Continuous glucose monitoring profiles in healthy nondiabetic participants: a multicenter prospective study. J Clin Endocrinol Metab. 2019;104(10):4356–64.
Tanaka H, Monahan KD, Seals DR. Age-predicted maximal heart rate revisited. J Am Coll Cardiol. 2001;37(1):153–6.
Canadian Association for Global Health C. Mesure de l’intensité de l’activité physique. 2012.
Marteau TM, Bekker H. The development of a six-item short-form of the state scale of the Spielberger State-Trait Anxiety Inventory (STAI). Br J Clin Psychol. 1992;31(3):301–6.
Wilkinson RT, Houghton D. Field test of arousal: a portable reaction timer with data storage. Hum Factors. 1982;24(4):487–93.
Hurdiel R, Peze T, Daugherty J, Girard J, Poussel M, Poletti L, et al. Combined effects of sleep deprivation and strenuous exercise on cognitive performances during The North Face(R) Ultra Trail du Mont Blanc(R) (UTMB(R)). J Sports Sci. 2015;33(7):670–4.
Miley AA, Kecklund G, Akerstedt T. Comparing two versions of the Karolinska Sleepiness Scale (KSS). Sleep Biol Rhythms. 2016;14(3):257–60.
Hurdiel RRS, Millet G, Mauvieux B, Pezé T, Elsworth-Edelsten C, Martin D, Zunquin G, Dupont G. Cognitive performance and self-reported sleepiness are modulated by time-of-day during a mountain ultramarathon. Res Sports Med. 2018;26(4):1–8.
Kaida K, Takahashi M, Akerstedt T, Nakata A, Otsuka Y, Haratani T, et al. Validation of the Karolinska sleepiness scale against performance and EEG variables. Clin Neurophysiol. 2006;117(7):1574–81.
Zinker BA, Mohr T, Kelly P, Namdaran K, Bracy DP, Wasserman DH. Exercise-induced fall in insulin: mechanism of action at the liver and effects on muscle glucose metabolism. Am J Physiol. 1994;266(5 Pt 1):E683–9.
De Feo P, Perriello G, Torlone E, Ventura MM, Fanelli C, Santeusanio F, et al. Contribution of cortisol to glucose counterregulation in humans. Am J Physiol. 1989;257(1 Pt 1):E35-42.
Klumpers UM, Veltman DJ, van Tol MJ, Kloet RW, Boellaard R, Lammertsma AA, et al. Neurophysiological effects of sleep deprivation in healthy adults, a pilot study. PLoS One. 2015;10(1): e0116906.
Jensen MD, Caruso M, Heiling V, Miles JM. Insulin regulation of lipolysis in nondiabetic and IDDM subjects. Diabetes. 1989;38(12):1595–601.
Roden M, Price TB, Perseghin G, Petersen KF, Rothman DL, Cline GW, et al. Mechanism of free fatty acid-induced insulin resistance in humans. J Clin Invest. 1996;97(12):2859–65.
Kirwan JP, del Aguila LF. Insulin signalling, exercise and cellular integrity. Biochem Soc Trans. 2003;31(Pt 6):1281–5.
Del Aguila LF, Krishnan RK, Ulbrecht JS, Farrell PA, Correll PH, Lang CH, et al. Muscle damage impairs insulin stimulation of IRS-1, PI 3-kinase, and Akt-kinase in human skeletal muscle. Am J Physiol Endocrinol Metab. 2000;279(1):E206–12.
Aoi W, Naito Y, Yoshikawa T. Role of oxidative stress in impaired insulin signaling associated with exercise-induced muscle damage. Free Radic Biol Med. 2013;65:1265–72.
Nieman DC, Dumke CL, Henson DA, McAnulty SR, Gross SJ, Lind RH. Muscle damage is linked to cytokine changes following a 160-km race. Brain Behav Immun. 2005;19(5):398–403.
Pedersen BK, Toft AD. Effects of exercise on lymphocytes and cytokines. Br J Sports Med. 2000;34(4):246–51.
Podlogar T, Wallis GA. New horizons in carbohydrate research and application for endurance athletes. Sports Med. 2022;52(Suppl 1):5–23.
Smith KA, Pugh JN, Duca FA, Close GL, Ormsbee MJ. Gastrointestinal pathophysiology during endurance exercise: endocrine, microbiome, and nutritional influences. Eur J Appl Physiol. 2021;121(10):2657–74.
Burr JF, Drury CT, Phillips AA, Ivey A, Ku J, Warburton DE. Long-term ultra-marathon running and arterial compliance. J Sci Med Sport. 2014;17(3):322–5.
Jafar O, Friedman J, Bogdanowicz I, Muneer A, Thompson PD, Ling J, et al. Assessment of coronary atherosclerosis using calcium scores in short- and long-distance runners. Mayo Clin Proc Innov Qual Outcomes. 2019;3(2):116–21.
Jung CH, Rhee EJ, Kim KJ, Kim BY, Park SE, Chang Y, et al. Relationship of glycated hemoglobin A1c, coronary artery calcification and insulin resistance in males without diabetes. Arch Med Res. 2015;46(1):71–7.
Muller J, Dahm V, Lorenz ES, Pressler A, Haller B, Grabs V, et al. Changes of intima-media thickness in marathon runners: a mid-term follow-up. Eur J Prev Cardiol. 2017;24(12):1336–42.
Radford NB, DeFina LF, Leonard D, Barlow CE, Willis BL, Gibbons LW, et al. Cardiorespiratory fitness, coronary artery calcium, and cardiovascular disease events in a cohort of generally healthy middle-age men: results from the cooper center longitudinal study. Circulation. 2018;137(18):1888–95.
Jeukendrup A. A step towards personalized sports nutrition: carbohydrate intake during exercise. Sports Med. 2014;44(Suppl 1):S25–33.
Ranchordas MK. Nutrition for adventure racing. Sports Med. 2012;42(11):915–27.
Tiller NB, Roberts JD, Beasley L, Chapman S, Pinto JM, Smith L, et al. International Society of Sports Nutrition Position Stand: nutritional considerations for single-stage ultra-marathon training and racing. J Int Soc Sports Nutr. 2019;16(1):50.
Kerksick CR. M. Supplements for Endurance Athletes. Strength Condition J. 2010;32:55–64.
Neubauer O, Reichhold S, Nics L, Hoelzl C, Valentini J, Stadlmayr B, et al. Antioxidant responses to an acute ultra-endurance exercise: impact on DNA stability and indications for an increased need for nutritive antioxidants in the early recovery phase. Br J Nutr. 2010;104(8):1129–38.
Tanabe Y, Fujii N, Suzuki K. Dietary supplementation for attenuating exercise-induced muscle damage and delayed-onset muscle soreness in humans. Nutrients. 2021;14(1):70.
Connolly DA, McHugh MP, Padilla-Zakour OI, Carlson L, Sayers SP. Efficacy of a tart cherry juice blend in preventing the symptoms of muscle damage. Br J Sports Med. 2006;40(8):679–83 (discussion 83).
Berger NJA, Best R, Best AW, Lane AM, Millet GY, Barwood M, et al. Limits of ultra: towards an interdisciplinary understanding of ultra-endurance running performance. Sports Med. 2023;54(1):73–93.
Bowtell J, Kelly V. Fruit-derived polyphenol supplementation for athlete recovery and performance. Sports Med. 2019;49(Suppl 1):3–23.
Howatson G, von Someren KA. The prevention and treatment of exercise-induced muscle damage. Sports Med. 2012;38(6):483–503.
Acknowledgements
The authors would like to thank the participants in this study. We thank J. Naturel and J. Lutun (Lille University) and V. Deprez and M-A Allain (Lille University Hospital) for their administrative support; J. Dereumetz (Lille University) for her help with data analyses; A. Bertrand (Statistical Methodology and Computing Service, UCLouvain, Belgium) for support with statistical analyses; and S. Platt (International Eyes SARL) for revising the English. We also thank A. Oliveira Alves and M. Osmont (Paris Cité University) for blood sampling and P. Pigny, F. Zerimech, and J. Demaret (Lille University Hospital) for blood analyses. Glycaemic analyses were carried out at the EURASPORT facility managed by S. Berthoin (Lille University).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This protocol was partly financed by the RIN TREMPLIN APEEX (Adaptation Physiologiques En Environnements Extrêmes – 2020/2022) supported by the Normandy Region – France and the European Regional Development Fund (ERDF). This study was undertaken as part of the project run by the International Joint Laboratory REGALE-1 (Glycemic Regulation During Exercise in Type 1 Diabetes), bringing together the URePSSS (Lille University) and IRCM (Montréal) and involving an international ‘SPORT-1’ Chair for R. Rabasa-Lhoret (I-SITE ULNE, WILL grant). This study was supported in part by grants from the Type 1 Running Team Association. EH received a grant from the Institut Universitaire de France, and CP received grant assistance as a doctoral student from the Hauts-de-France Regional Authority.
Competing Interests
The authors declare no competing interests.
Ethics Approval
Approval institution, Ouest III Ethics Committee; ethics number, 2021-A01765-36; date of approval, 26 October 2021. Trial registration number, NCT05538442 2022-09-21, retrospectively registered. The study was performed in accordance with the ethical standards in the Declaration of Helsinki.
Consent to Participate
All participants were fully informed of the nature and possible risks of the experimental procedures before their written informed consent was obtained.
Consent to Publication
Not applicable.
Code Availability
Not applicable.
Authors’ Contributions
All authors read and approved the final version. EH and BM designed the experiments. FXG and RRL gave advice on some methodological points. CP, EL, EH, JCV, RH, PLD, SB, PN, VG, PB, QM, and RJ carried out the experiments and collected the data. PM performed blood analyses. EH and CP analysed the data. JH created algorithms for analyses of glycaemic excursions and variability. BM and CH recruited the participants, organized the protocol and the race, and submitted the protocol to the ethics committee. EH and CP wrote the manuscript. All authors were involved in reviewing the manuscript. EH has guaranteed the integrity of the study throughout its duration and, as such, had full access to data and takes responsibility for the integrity of the data and accuracy of the data analysis.
Data Availability Statements
All data related to this article are available on http://www.data.gouv.fr/fr/ platform (https://doi.org/10.57745/EO2SBC).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Parent, C., Mauvieux, B., Lespagnol, E. et al. Glycaemic Effects of a 156-km Ultra-trail Race in Athletes: An Observational Field Study. Sports Med (2024). https://doi.org/10.1007/s40279-024-02013-4
Accepted:
Published:
DOI: https://doi.org/10.1007/s40279-024-02013-4